
Olivia Bottazzini
Olivia Bottazzini (she/her) has completed her final semester at Capilano University and will graduate in January 2026 with a Bachelor of Arts majoring in Interdisciplinary Studies. Olivia received high marks throughout her studies and was on the Dean’s List for her last two years at Capilano University for this dedication. Olivia decided to pursue teaching in high school while volunteering at an East Vancouver Elementary School. Olivia has built strong ties to the community over the past two years through her elementary school tutoring service and will continue to tutor post-graduation. Olivia hopes to begin a professional teaching degree after graduation and then begin a career as a teacher. Olivia is looking forward to working in the classroom with students when she completes her teaching certificate.
High school students must receive an in-depth sexual health education in order for them to make informed decisions regarding contraception. Although students may learn about their sexual health elsewhere, “where adolescents get their sexual health information is important” (Rotermann and McKay 4). Sex educator Alexander McKay and academic researcher Michelle Rotermann’s paper, “Where Do 15- to -17-Year-Olds in Canada Get Their Sexual Health Information?” analyzes data describing how the youth are learning about sexual health. Among the students researched in Canada, the leading ways they are obtaining knowledge about sexual health is through their schools, parents, and the internet (7). While 55.6% of students learn about sexual health in school and 51.2% of students from their parents, 45.9% of students are using the internet as their source (7). While the internet is not the leading source for students, this statistic is concerning regardless because “quality and accuracy [is] not always as high” (3). With a more comprehensive high school sexual health education curriculum, we can prevent students from using unreliable sources and focus on their knowledge coming from school.
My Personal Recollection
I remember first learning about contraception in my tenth-grade physical education class in 2017. My teacher took us to a local youth sexual health clinic, and there, the nurses briefly outlined each contraceptive method available at the time. I recall learning about the reasoning behind the use of contraceptive methods, the efficacy of each method, and where we students could access this contraception. With this class in mind, I returned to the clinic about a year later to seek out a prescription for the birth control pill. I was on the pill for just over a year before learning from my family doctor that it was dangerous for me, someone who has high cholesterol and a family history of heart problems. I remember feeling frustrated that after all these months of taking this contraceptive method, I was unaware of the risks. After going off the pill and speaking with my doctor, we decided that an intrauterine device (IUD) would be best suited for me. I was not fully informed of the steps of the IUD insertion process, nor was I aware of the possibility of severe pain during the procedure. This led to the insertion process being a traumatizing experience where I felt misled and betrayed. Had British Columbia’s sexual health education curriculum been more detailed, I would have been properly informed before taking the birth control pill and getting an IUD.
Usage of Hormonal Contraceptives
My negative experiences with hormonal contraceptive methods are not unique. In 2021, there were approximately 253,690 youths in British Columbia (BC) between the ages of fifteen and nineteen, a number that has likely since increased (“Census Profile, 2021: Census of Population Profile Table”). We have an extensive population of adolescents in BC, and for many young people, hormonal contraceptive prescriptions may be their first experience with prescription medication. To ensure that students can make voluntary decisions when it comes to selecting their contraceptive methods, their education must effectively prepare them. What if sexual education in high school were improved? What if, rather than solely explaining that contraceptive methods prevent pregnancy to students, they were provided with more in-depth knowledge? What if BC’s youth were told about the side effects, procedures, and possible contraceptive methods to avoid depending on the individual? As someone who has experienced using multiple forms of hormonal contraception, I would have benefited from a better understanding of this topic as a young teenager. If the high school curriculum were to clearly outline to educators what needs to be taught, both students and teachers would be helped because they would be knowledgeable about the importance of hormonal contraceptive education. For there to be a consistent understanding of students about hormonal contraception across BC, the curriculum needs to be specific, including the efficacy, side effects, procedures, and information on contraceptive methods to avoid depending on medical conditions and medications. A comprehensive sexual health curriculum will ensure that students are able to make informed decisions about contraception, specifically hormonal contraceptive methods.
Hormonal contraception can be presented as a simple solution, but individuals need to fully consider their contraceptive options before making decisions. Hormonal contraceptive methods consist of either progestin, or a combination of progestin and estrogen to prevent pregnancy (“Hormonal Birth Control Methods” par. 1). The birth control pill, patch, shot, vaginal ring, implant, and the hormonal intrauterine device (IUD), are all examples of hormonal contraceptive methods that come with possible side effects on the body (“Hormonal Birth Control Methods”). Individuals taking hormonal contraceptive methods may not experience any side effects; however, there are possible risks with each method (Catlett).

This is an image of the contraceptives aisle at a Superstore on the North Shore. This picture shows how overwhelming looking at contraceptive method options can be, as there are dozens of condom varieties here. For someone unaware of the different contraceptive methods, they may think this is all that is available.
In nurse practitioner Kelley S. Borella and pharmacist Shareen Y. El-Ibiary’s article titled “Continuing Education: Exploring the Latest Developments in Hormonal and Nonhormonal Contraceptive Options,” the authors highlight the possible side effects for individuals using various progestin and combination contraceptive methods. The side effects of taking progestin pills include acne, headaches, bloating, changes in libido, dizziness, and an increased appetite, which can lead to weight gain (Borella and El-Ibiary 6). For individuals taking combination birth control pills, possible side effects may differ, including mood fluctuation, irregular bleeding, weight gain, headaches, and a decreased libido (7). The vaginal ring can lead to headaches, irregular bleeding, and nausea, whereas the patch may cause rashes and acne (8). Individuals with IUDs may experience abnormal bleeding, cramping, and a possibility of ovarian cysts forming (9). When speaking about the implant and shot, physician Nancy Grossman Barr explains that the implant can bring on irregular bleeding, and individuals with the birth control shot can also experience this irregular bleeding, as well as weight gain and depression (1499, 1503). Due to the listed side effects for each contraceptive method, individuals must be well-informed prior to using these methods.

This is a photo of me holding up an information sheet that comes in a birth control pill box. As you can see, it is the length of my torso, and the entire front side of the paper is in English. For a young teenager, this information can be overwhelming and will likely not be read. The sheet contains information on the efficacy, ingredients, side effects, and usage.
BC High School Curriculum and Hormonal Contraceptives
The current high school sexual health education curriculum is vague in that there are general guidelines, but no specific details that must be covered. On November 11, 2025, I interviewed a North Shore physical education teacher of twenty years, whom I will call Ms. Smith for the purpose of this study (“Interview with an anonymous teacher”). She explained that BC’s curriculum highlights topics like, “Puberty, anatomy, healthy relationships, consent, sexual decision-making, and preventing unintended pregnancy and Sexual Transmitted and Blood Borne Infections (STBBIs).” Contraception is discussed in tenth-grade classrooms in the “Healthy Sexual Decision Making” unit in sexual education (Ministry of Education and Child Care 24, 40). Numerous sex-related topics are covered in sexual health education; however, the curriculum does not describe what needs to be taught for each subject, but rather it states topics like “anatomy” and “sexual decision-making.” With there being several possible side effects to using hormonal contraceptive methods, the curriculum should require that teachers educate their students on specific information when it comes to these methods. Not only would students receive a more comprehensive understanding of hormonal contraception, but teachers would benefit from knowing exactly what is to be taught.

This is a picture of a gym in a high school on the North Shore. For tenth-grade students learning about their sexual health, this will likely be the location of the teaching.
With the current BC sexual health curriculum being extremely vague, there is the possibility of educators imposing their own moral beliefs into their teaching, for example, not including certain contraceptive methods. In Canadian journalist Akhila Menon’s article, education experts explain in a Tyee interview that teachers in BC schools are obligated to teach sexual health education to students in kindergarten, up until the tenth grade (par. 17). Although there may be a requirement for this teaching, interviewees clarify that what is being taught depends on the teacher and district (Menon par. 21). For teachers in BC, there is a lack of training given on sexual health education, other than suggested resources (par. 39). When teaching materials are left up to school districts, schools, and educators, there can be an inconsistency in the information distributed across schools. Sexual health educator Saleema Noon discussed in the Tyee interview that while some teachers may appreciate this broad approach to sex education in BC, others may struggle (par. 39). A teacher’s understanding of “preventing unintended pregnancy” may vary depending on their personal views, and Menon’s article uncovers that conservative approaches focusing on abstinence rather than detailing contraceptive methods can be seen in parts of BC, such as Langley and Abbotsford (par. 22). One can argue that abstinence should be touched on in classes, as long as other contraceptive methods are also discussed. When teaching students about these methods to prevent pregnancy, educational resources can be useful.
A solution to teaching comprehensive sexual education can be educational resources like Sex Sense. Sex Sense is a free sexual education resource in BC. I had the opportunity to speak to Robin from Sex Sense about sexual health education in BC. Robin affirmed my understanding that high school sexual education is broad, and as of now, teachers are not receiving a detailed description of what is to be taught to students. Through my conversation with Robin, I also discovered that teachers are not required to have any specific knowledge of sex education before beginning to teach this topic. This can be problematic as students’ education will be based on a teacher’s level of interest and knowledge of the topic. Also, during our conversation, Robin discussed Sex Sense as a tool for schools. Rather than schools having physical education teachers or other educators from the school inform students about sexual health education, there are useful companies such as Sex Sense (Robin). When speaking to anonymous teacher Ms. Smith in our interview, she explained that at the school where she works, an organization similar to Sex Sense teaches sex education. However, she mentioned that the school district funded this resource. Therefore, students in school districts that are unable to afford organizations like Sex Sense will not receive this teaching.
Not all students have had access to organizations like Sex Sense. Brittany, a twenty-three-year-old woman, revealed that while my class went to a sexual health clinic nearby, hers did not, and this was her teacher’s choice (Brittany). This impacted her education on sexual health. Brittany has been using hormonal contraception since she was fourteen years old. Although she has used the combination birth control pill, the progestin pill, and the Depo-Provera shot, her understanding of these methods did not come from high school. Brittany clarified that during sexual health education lessons, the contraceptive methods that were primarily spoken about were condoms and abstinence, and little detail was given when discussing hormonal contraception. She recalls that the educator stated that contraception prevents pregnancy; however, there was no discussion on how the methods work and how one’s body may respond. Brittany used the internet to obtain an understanding of her contraception options, but when Brittany began using contraceptive methods, she struggled to find a method that worked with her body. The many different pills that she tried worked at first, and then would suddenly stop working, and she experienced abnormal bleeding. When she tried the birth control shot, she experienced irregular bleeding for nearly six months afterwards. She continued to use the internet to help gain an understanding of why her body was reacting this way, when she was told by health professionals that these were simply side effects. Brittany feels that high school should have prepared her better. Brittany urges that had she learned more about these hormonal contraceptive methods in high school, she explains, “I would have a more positive stance on birth control methods because I would be prepared, instead of me having a blind approach to trying them.”
Brittany is not the only student who has had negative experiences with sexual health education. I interviewed a student on November 12, 2025, who would prefer to remain anonymous, and she will be referred to as Sarah (“Interview with an anonymous student”). Sarah graduated from a high school on the North Shore in 2019, and she expressed that she was not taught about contraception in her studies. Sarah remembers an inconsistency in sexual health education across her school. While some of her peers in other classes were learning about contraceptive methods, Sarah’s class did not, and as a result of this, her knowledge came from the internet and her friends. She felt as though she did not know where to get reliable information about sexual health. Had she been taught about contraceptive methods in her sexual health classes, Sarah states, “I would have felt a lot more confident and in control of my own choices about sexual health.”
BC Curriculum: Attitudes and Proposed Changes
It is beneficial for students that their understanding of sexual health comes from school rather than the internet, and improving the current curriculum is necessary. During an interview with a sexual health educator at The University of British Columbia, Kristen Gilbert, she explained that the entirety of BC’s curriculum is far from specific. Rather than each subject going into extreme detail about what is to be taught, general topics are highlighted (Gilbert). When talking about the curriculum, Gilbert stated, “It gives general or broad guidelines which empower the teacher… to use their knowledge and skills to develop content.” While this broadness may be useful for teachers educating students on other subjects, there needs to be more specific criteria when it comes to sexual education to ensure that students leave high school with a proper understanding of sex related topics, and of their autonomy. Gilbert also heard my idea that sexual education should be more comprehensive. She suggests that, rather than teachers discussing these topics that they may be unfamiliar with, they direct students to speak with clinicians. Although I agree that teachers should have the professional autonomy to teach what they are comfortable with, not every adolescent is able to meet with a clinician.
For young individuals, speaking to clinicians is not always easy. Some individuals may struggle with opening up about their sexual health, and in addition, resources like clinics are not always available. Students from West Vancouver, such as myself, may be directed to the West Sexual Health Clinic, a place where youths can get free contraceptive methods and other services (“West Sexual Health Clinic”). It is necessary to highlight that this clinic is only open on Tuesdays from 2:15 pm-4:30 pm; therefore, if an individual does not want to leave class early, they will likely not see a clinician, and accessing appointments with general practitioners can be difficult as well.
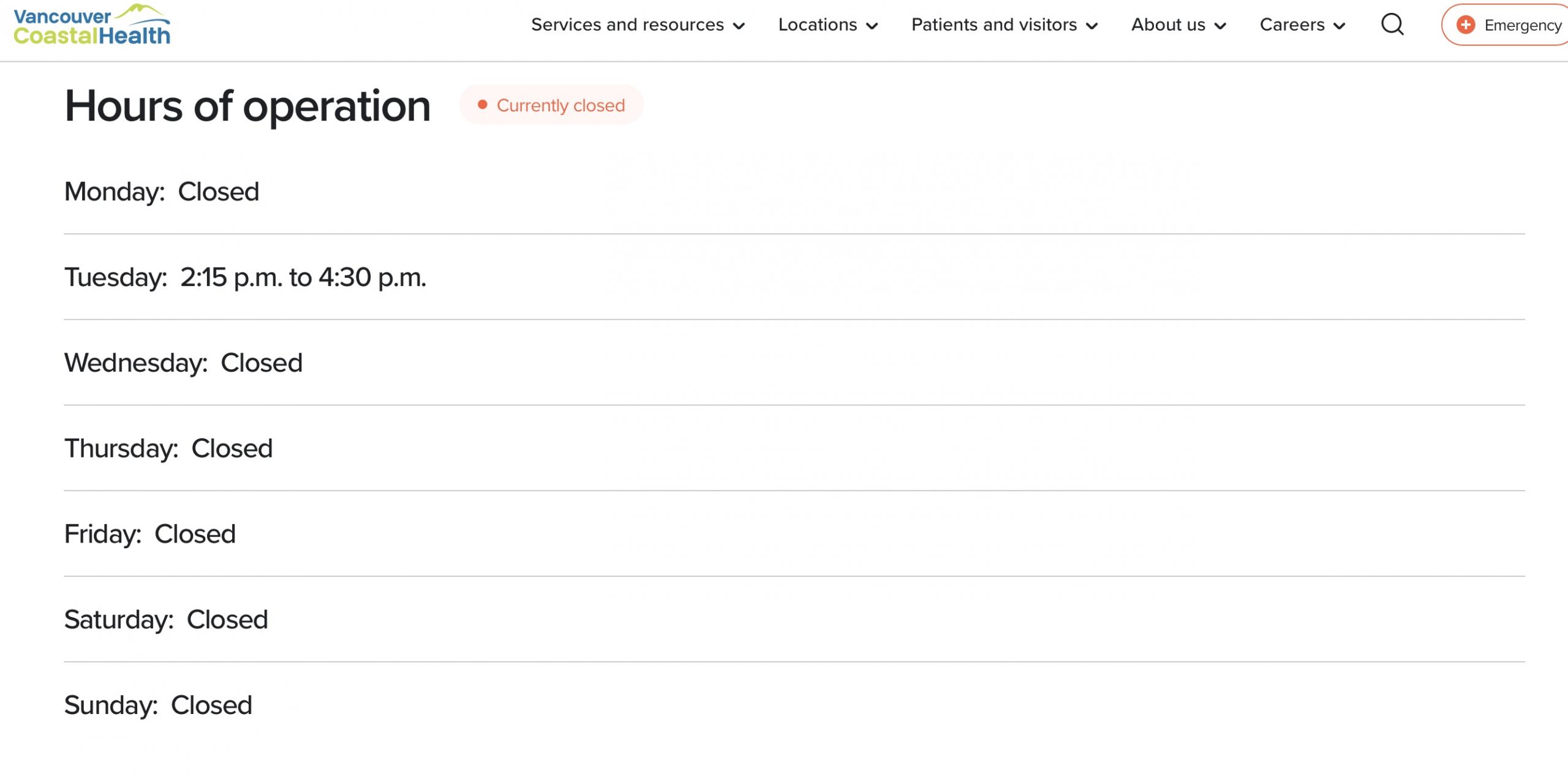
This is a screenshot of the West Sexual Health Clinic’s hours in West Vancouver. As you can see, the clinic is only open for just over two hours a week. If a student wants to see a clinician, they will likely have to leave school early, which will interfere with their classes.
Individuals across BC may believe that the teaching of sexual education to youth is not up to high schools, but rather, it should be taught by general practitioners. Although I can agree that students would benefit from being taught about sexual health from health professionals themselves, this is sadly not possible as we are in a “family doctor crisis” in BC (Kurjata par. 34). In his CBC News article, producer and reporter Andrew Kurjata contextualizes that nearly 400,000 people across BC do not have access to a general practitioner (par. 15). After speaking to HealthLink BC, a free phone service that allows people to join the family doctor waitlist, people are typically quoted up to a year or more when signing up to be on BC’s general practitioner waitlist (HealthLink BC). Additionally, individuals who have access to general practitioners are not always comfortable discussing their sexual health. My family doctor is a man in his sixties, and as a twenty-three-year-old woman, I often feel uncomfortable discussing matters relating to my body and my sexual health. Rather than an intimidating one-on-one conversation with a general practitioner, classroom sexual health education lessons create a more comfortable situation for students.
In order to determine whether I believe improving the sexual health curriculum in BC is possible, I spoke to the anonymous teacher Ms. Smith about how she has observed the curriculum changing. Ms. Smith explained that when she was in high school, approximately thirty to forty years ago, the only information students were shown regarding sexual health was a video showing a woman giving birth. While she has been teaching physical education over the past twenty years, Ms. Smith has noticed a changing curriculum, particularly in the past eight or so years, now highlighting what she calls, “A physical and health education focus.” The evolutionary change of BC’s sexual health education curriculum showcases that improvements are possible, and a more comprehensive curriculum may be in BC’s future if this is prioritized.
While curriculum improvement is a possibility, the importance of sexual health needs to be collective; schools must recognize this, but parents too. In 2020, there was a Canada-wide study that looked at whether parents believe sexual education should be taught to their children in school, and 90% of parents agree with this statement (Menon 68). To understand the remaining 10% of parents’ take on sexual health education, we can look at a study conducted in the United States. Researchers Jeffrey L. Hurst et al. concluded in their study that the parents who see sexual education as a low priority for their child tend to be those with politically conservative views and/or very religious beliefs (121). Although this study fails to speak to Canadian parents, this may be a North American trend, and these conservative and religious views on sexual education must be considered. A common misconception is that sexual health education in high school will influence students to have sex, and an educational resource created by the United Nations Educational, Scientific and Cultural Organization challenges this, explaining that, instead, proper sexual health education lowers both the frequency and initiation of sexual behaviours (28). In addition, sexual health education increases contraceptive use (UNESCO 28). In a study looking at whether individuals used contraception the last time they participated in sexual activity, described by Statistics Canada analyst Tia Carpino, young people’s usage was higher (par. 8). The study took place in 2019-2020, and fifteen to twenty-four-year-olds reported contraceptive use for 89.6% of individuals, over 5% higher than the twenty-five to thirty-four age group (Carpino par. 8). This da2ta makes it clear that contraceptive methods are being used by young people, and these individuals are more likely to make informed decisions with a proper understanding of their preferred contraceptive methods.
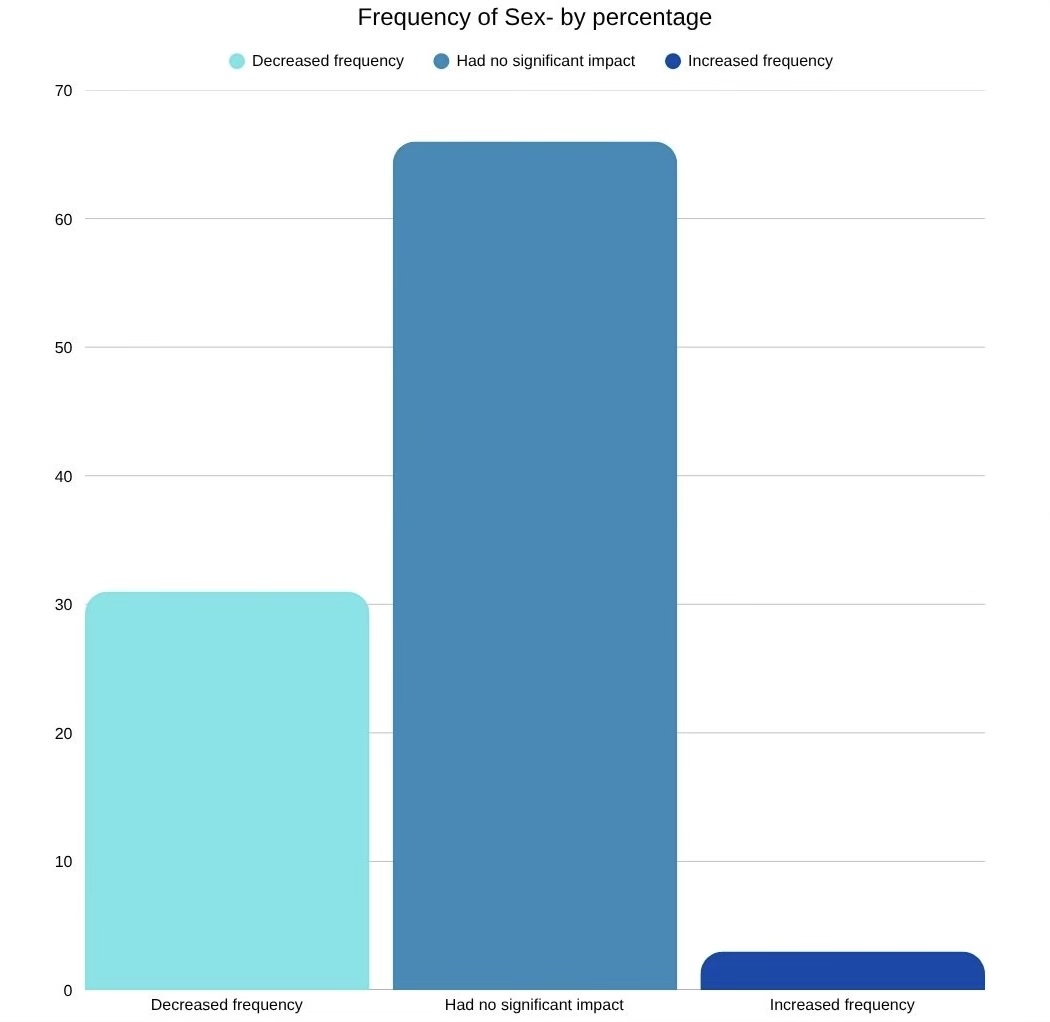
This is a bar graph I created that shows the United Nations Educational, Scientific and Cultural Organization’s data on how high-quality sexual health education influences the frequency of sex (UNESCO 128). According to the data, sexual education primarily decreases the frequency of sex, or does not impact it, rather than increasing the frequency.
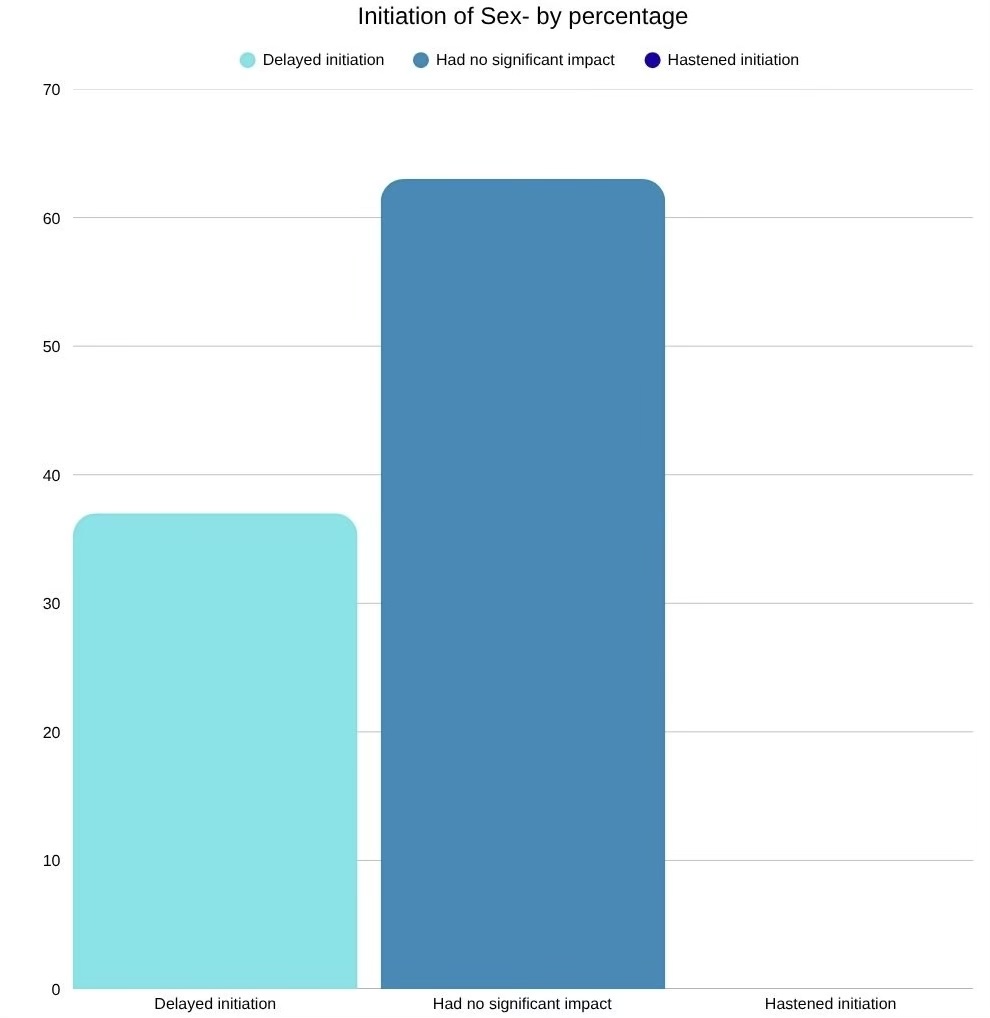
This is another bar graph that I put together that highlights how high-quality sexual health education can impact the youth’s initiation of sex (UNESCO 128). The data comes from the United Nations Educational, Scientific and Cultural Organization’s resource on sexual education. The chart shows that for most individuals, sexual education delays or does not impact initiation.
To ensure that youth in BC can make informed decisions regarding hormonal contraceptive methods, the curriculum must include procedures, efficacy, side effects, and ways these methods may interact with medications and medical conditions. If teachers receive adequate training on how to educate their students on hormonal contraceptive methods, and the curriculum outlines what specifically needs to be taught, students as well as teachers will benefit from consistency across the province. If I had known more information before taking the birth control pill and getting an IUD, I would have had a better experience with hormonal contraception. Continued research on hormonal contraceptive methods is necessary to keep youth up to date during their sexual health education lessons.
Works Cited
Borella, Kelley S., and Shareen Y. El-Ibiary. “Continuing Education. Exploring the Latest Developments in Hormonal and Nonhormonal Contraceptive Options.” Women’s Healthcare: A Clinical Journal for NPs, vol. 12, no. 1, Feb. 2024, pp. 4–10. EBSCOhost, https://doi-org.ezproxy.capilanou.ca/10.51256/WHC022404.
Brittany. Interview. 28 October 2025. Telephone interview.
Carpino, Tia. “Contraception Use among Sexually Active Women Wanting to Avoid Pregnancy.” Statistics Canada, Statistics Canada, 10 Feb. 2025, www150.statcan.gc.ca/n1/pub/45-20-0002/452000022025001-eng.htm.
Catlett, Tess. “The Effects of Hormonal Birth Control on Your Body.” Healthline, Healthline Media, 24 Feb. 2024, www.healthline.com/health/birth-control-effects-on-body#sexual.
“Census Profile, 2021: Census of Population Profile Table.” Statistics Canada, Statistics Canada, 2021, www12.statcan.gc.ca/census-recensement/2021/dp-pd/prof/details/page.cfm?Lang=E&SearchText=British%20Columbia&DGUIDlist=2021A000259&GENDERlist=1.
Gilbert, Kristen. Interview. 7 November 2025. Email interview.
Grossman Barr, Nancy. “Managing Adverse Effects of Hormonal Contraceptives.” American Family Physician, vol. 82, no. 12, Dec. 2010, pp. 1499–506. EBSCOhost, research.ebsco.com/linkprocessor/plink?id=42e8a580-822e-3143-90ea-0120ac72acc8.
HealthLink BC. Personal communication. 6 November 2025. Telephone.
“Hormonal Birth Control Methods.” Action Canada for Sexual Health & Rights, Action Canada SHR, www.actioncanadashr.org/sexual-health-hub/hormonal-birth-control-methods.
Hurst, Jeffrey L., et al. “Parents’ Attitudes towards the Content of Sex Education in the USA: Associations with Religiosity and Political Orientation.” Sex Education, vol. 24, no. 1, Jan. 2023, pp. 108–24, https://doi.org/10.1080/14681811.2022.2162871.
Kurjata, Andrew. “B.C. Has Recruited Hundreds of Family Doctors. It’s Still Not Enough.” CBC, CBC/Radio-Canada, 21 Mar. 2025, www.cbc.ca/news/canada/british-columbia/family-doctor-recruitment-shortage-2024-1.7489398.
Menon, Akhila. “Sex Education in BC’s Schools: An Explainer.” The Tyee, Jeanette Ageson, 9 Dec. 2022, thetyee.ca/News/2022/12/09/Sex-Education-BC-Schools-Explainer/.
Ministry of Education and Child Care. “Supporting Student Health Guide: Secondary.” British Columbia, 2022, curriculum.gov.bc.ca/sites/curriculum.gov.bc.ca/files/pdf/subject/phe/Supporting_Student_Health_Secondary.pdf.
Robin Sex Sense. Personal communication. 6 November 2025. Telephone.
Rotermann, Michelle, and Alexander McKay. “Where Do 15- to -17-Year-Olds in Canada Get Their Sexual Health Information?” Health Reports, vol. 35, no. 1, Jan. 2024, pp. 3–13. EBSCOhost, https://doi-org.ezproxy.capilanou.ca/10.25318/82-003-x202400100001-eng.
UNESCO. “International Technical Guidance on Sexuality Education an Evidence-Informed Approach.” United Nations Educational, Scientific and Cultural Organization, UNESCO, 2018, www.unfpa.org/sites/default/files/pub-pdf/ITGSE.pdf.
“West Sexual Health Clinic.” Vancouver Coastal Health, Vancouver Coastal Health, 2025, www.vch.ca/en/location-service/west-sexual-health-clinic.
Interview with an anonymous teacher. 11 November 2025. Email interview.
Interview with an anonymous student. 12 November 2025. Email interview.
