Our shared capacity grows in somatic and compassionate practice.
“Your river of feelings might feel like it’s flowing over you, but actually you’re the river’s source.”
—Lisa Feldman Barrett, How Emotions Are Made: The Secret Life of the Brain, 2017

Sheena Venditti
Sheena Venditti (she/they) gratefully and humbly recognizes that they are a settler speaking, living and learning on the unceded, ancestral, and occupied, traditional lands of the xʷməθkʷəy̓əm (Musqueam), Səl̓ílwətaʔ (Tsleil-Watuth), Stó:lō, Shíshálh (Sechelt) and Skwxwú7mesh (Squamish) Nations of the Coast Salish peoples.
Sheena will complete their journey at Capilano with a Bachelor of Arts in Psychology in the spring of 2026 and is eager to begin Master of Counselling training in the coming year. Inspired by experimental research aimed at better describing group motivation as well as applied research projects undertaken with public and NGO partners during her undergrad, Sheena hopes to engage in the delivery and facilitation of group therapies in her future career, while continuing to contribute to her ongoing volunteer and advocacy work.
The air is cold, almost shocking, as I push the side door from the kitchen open. I had been sweating from the final hustle to tidy up the dishes—80 people ate with us tonight, and our tiny dishwasher had made the space a sauna. “Night! Love you guys, see you next time…”
I let the door slam behind me and took a few broad strides toward my car, feeling a wonderful sense of rest, a deep settling wash over me as I popped the trunk. Three years ago, I couldn’t stand chopping vegetables for more than a few hours before I had to draw on my energy reserves just to drive home. Tonight, I ran all over that hall for seven straight hours, and now I’m vibrating with more energy than I started with, solid on my feet. This all took practice. I needed to practice relating with value-aligned communities and being open to vulnerability to gain real resilience.
There is a significant difference between “not traumatized” and living well. That space is bridged by awareness of the relationships we create in our shared spaces—what I call community care. We foster community care by collaborating with people to create something durable within our community, taking action to contribute to others. This builds our individual capacity and our shared survival.
Lacking Capacity
After nearly losing my life in a boat accident in 2019—ricocheting around a vehicle at 70 kilometres an hour—I found that some parts of my body would never totally recover. I had to face up to the reality that some of what I thought was possible for me in the future was now impossible. At the conclusion of my official rehabilitation, I was terrified and ashamed. I had met all the insurance marks to return to work, but the time it took to care for those injuries and manage stress symptoms continuously outpaced the hours in the day when a full work schedule was also required. It was not possible to complete both.
A personal photo taken from a doctor’s office: the MRI results before my first emergency surgery in August 2019. By Sheena Venditti, October 2020.
I could no longer physically perform in a “competitive” manner. My decade of training in carpentry and my twenty years in commercial kitchens seemed useless as I struggled just to stand and walk for an hour straight. All my hobbies—kayaking, snowboarding, backcountry camping, surfing—were things my physiotherapist said I could return to with good health maintenance. But I was struggling to keep up with that upkeep while managing my work duties.
My social time usually involved people asking how I was doing, listening to a summary of my situation, then quickly telling me I was lucky to be alive while desperately hoping for something less terrible to spark further conversation. It was easy to imagine that even those close to me felt burdened by my presence; I knew I made them uncomfortable. Medical treatments taught me how to manage the body I was left with, but those efforts alone couldn’t fully restore my understanding of what these changes meant, how they felt. When my body changed dramatically, I had to rebuild not only my physical capacity but also my understanding of who I was in this world, because my motor senses were receiving entirely new signals. How others responded to my movements, how it felt to move, what emotional faces I saw in their reactions to me—these social concepts were colliding in ways I had not yet understood.
This is not an uncommon experience. Research from the Institute for Work & Health shows that among 1,132 people who experienced an injury that removed them from work, 39% would not describe themselves as flourishing eighteen months later (Dobson et al., 2024). More disturbingly, a study of almost 20,000 people found that patients were 40% more likely to be hospitalized with a mental health diagnosis in the year after a major trauma (Leung, 2018). These statistics point to a social rupture that occurs when people find themselves outside of social connections and meaningful roles in their communities. Following evidence-based strategies alone to repair what ails us can rupture our sense of belonging and push us further from social connection.
Why does this happen? When we face trauma, our autonomic nervous system shifts into defensive survival mode, and the ability to rest and recover shuts down in response to continuous sensing of stressful uncertainty. Bio-neurologist Stephen Porges’ polyvagal theory contends that self-soothing is not sufficient to recover from these threatened states; we have to get into connection to achieve “neuroception of safety,” or co-regulation—the unconscious detection of safety felt with others (Porges, 2025). Lisa Feldman Barrett’s research on how emotions are constructed helps clarify why this is profound: our brains actively construct our perceptions and emotions through prediction and sensation experience. We unconsciously remember what to expect in any context, with all embodied information directing us to determine how we should feel. Barrett explains: “We learn emotional concepts from culture—including which body signals to suppress” (Barrett in Huberman Lab podcast, 2023).
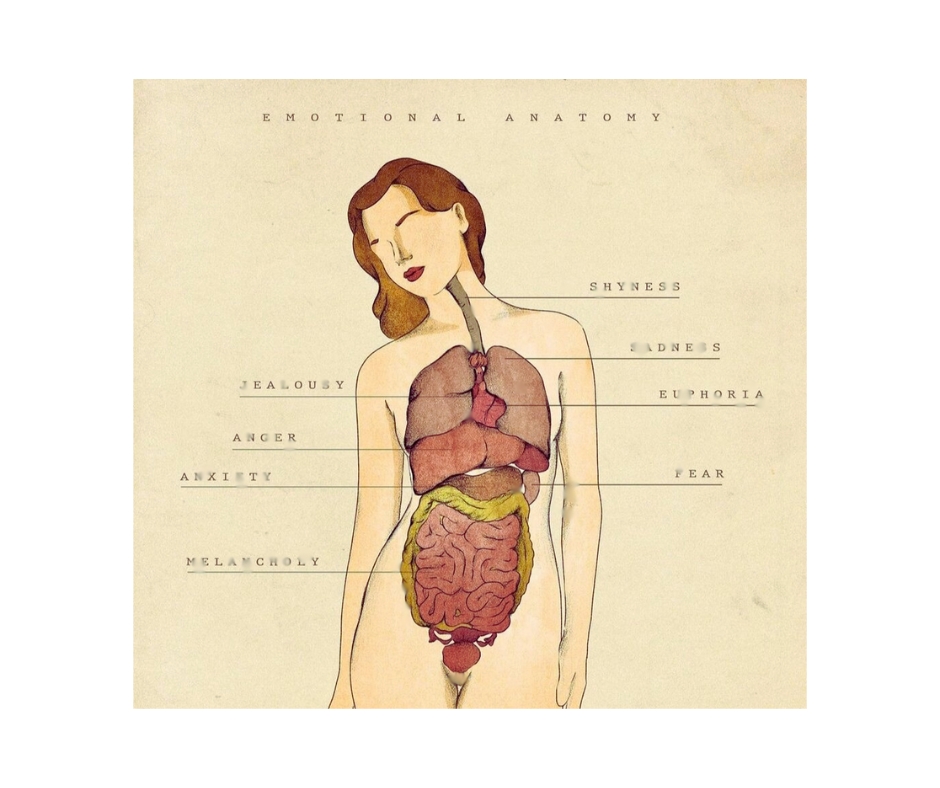
Some believe we store unprocessed emotions in parts of the body: an artistic rendition. From “Emotional Anatomy,” by Giulia Rosa, n.d., https://stay-hop.com/products/emotional-anatomy?_pos=1&_sid=45706d293&_ss=r.
Healing justice practitioner Prentis Hemphill, who has worked extensively with Black Lives Matter and grassroots movements, teaches somatic embodiment—the practice of being fully present in our bodies and relationships. For Hemphill, this means “to be intentional about what it is that we do, act, risk—how we connect. It’s the awareness of the real subtleties of how we feel. It’s the awareness of what we’ve stored and learned and then the promise of what we can be when we really center the body” (Hemphill in Loehnen, 2024).
Psychologist Kristin Neff’s research on self-compassion clarifies what this presence requires: recognizing our common humanity, treating ourselves with kindness rather than harsh judgment, and maintaining mindful awareness of our suffering without over-identifying with it (Neff & Germer, 2018). Practicing somatic embodiment means bringing awareness to the complex shifts in our bodies to better name how we can respond to the world, honouring our own needs and limits, and being brave enough to share those experiences in our relationships (Hemphill, 2024). Can we learn to struggle and feel uncomfortable alongside the people in our lives, giving them space to feel what is true for them without trying to fix it?
When my recovery wasn’t going well, when I was scared and ashamed, I asked for help. I started asking my care team for recommendations for support groups. After learning how to share how I was really feeling in those spaces, I wanted to tell others about the skills and resources I had gained. The more curious I got, the more care I received, the more resourced I became.
Eventually, I developed a solid practice of caring for my experience; I became better at accepting what was real for me and my capacity with more gentle awareness. I wanted to start putting myself out there for new experiences and testing my growing skills when a friend invited me to volunteer at an outdoor community movie event. I almost said no; I was worried I would be an inconvenience or make more work for others. But something about “just show up, do what you can” felt different from the all-or-nothing demands of work. The first night, I could only help for an hour before exhaustion hit. No one commented. Someone offered me water, we talked as I rested, and I relaxed my automatic response to ‘prove’ myself in this space. It’s these small experiences of engagement without evaluation that can shift how we understand ourselves.
Standing in that cold parking lot three years later, feeling strength in my legs, I recognized what actually helped me heal. It wasn’t just surgery and physiotherapy, though those mattered. My body had learned, through repeated somatic experience, that safety could exist in connection, that vulnerability wasn’t danger but a doorway. These stories reflect what I discovered when I chose to cross that threshold.
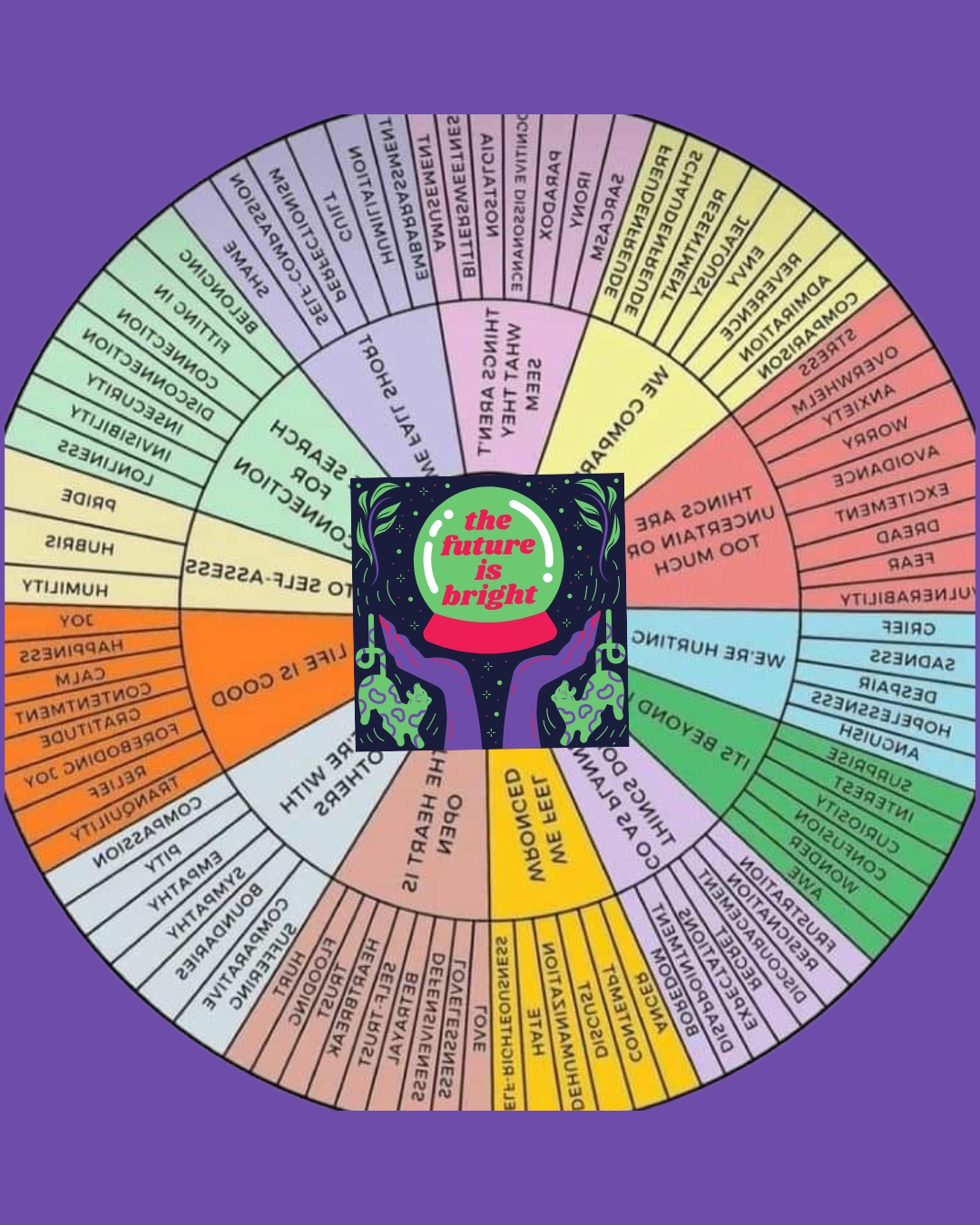
We utilize prediction and our current situation to determine the feelings we should express and how safe we are to prompt them.
A crystal ball imbedded in a therapy resource for naming feelings. Illustration of a crystal ball from “Think positive,” by CognitoCreative, 2020, https://tinyurl.com/yc56xryz. Background image adapted from “Emotions wheel feelings chart resources,” by KnowtheFundamentals, October 2025, https://tinyurl.com/yser8bnn.
When Following the Rules Fails, Make New Rules
Suzie, a Montreal-born creative and self-described weight-cycler has spent most of her life listening to expert advice on how to tame her “unruly body.” Suzie’s story clarifies something mine only hinted at: how thoroughly we’re trained to distrust our own sensations, and how we override our bodies and emotions in favour of external measures.
In 2013, the then 37-year-old MAC makeup artist entered what her community celebrated as a health challenge, aimed at losing significant weight through intensive exercise and strict dietary control, all of which was regularly reported in the local newspaper. She lost over half her body weight in eighteen months, continuing intense training long after the challenge concluded. When I asked if she ever felt conflict between the rules she was following and what her body was telling her, the response was immediate: “Yes! There are these ridiculous idioms that I repeated to myself, like ‘when you’re hungry, those hunger pangs, those are just the feeling of fat leaving your body.’ Never did it occur to me that it could also mean that I was just hungry,” (personal communications, interview, Oct. 30, 2025).
Ignoring her body’s hunger signals was necessary to meet dictated goals. Porges is familiar with this starting point: “Often we have been taught, as part of a strategy to manage our behaviour, to reject the feedback that our body is telling us,” (Porges, 2017, p. 50).
During this transformation, Suzie became aware of the growing body-liberation movement. Seeing her “old self” discussed in nuanced ways, praised even, created emotional dissonance. She pressed on partly because: “My mental health was directly correlated to the number on the scale. If it were moving down, I was good. But as soon as I stepped on the scale and it was the same or up a little, it was absolutely torment for me. And the more I lost, the more I was celebrated.”

Suzie’s publicized weight loss challenge: a collage of the intimate details that were broadcast on her journey. Images adapted from Times Colonist Victoria articles and Suzie Spitfyre’s personal blogs, design by Sheena Venditti, November 2025.
When repeated injuries to her surgically repaired ACL forced her to stop training in late 2016, she lost connection to the fitness communities she’d belonged to, Suzie recalls: “I was mad at my body. I was mad at myself. I was doing all the things I was supposed to be doing. And, I was like, ‘Why are you not cooperating?’”
Rather than cultivating present-moment awareness or curiously sensing what her body needed, Suzie had learned to treat her body as an object. Her well-being was expressed through her ability to be controlled, to demonstrate discipline, and to comply with what her trainers deemed good. She wrote on her blog in 2020: “…tired of being ashamed, embarrassed, angry, and bitter, of avoiding things, of isolating myself, I was scared of who I’d become, and of what people thought of me” (Spitfyre, 2020).
The turning point came when a friend invited Suzie to a women’s circle where sharing meant simply witnessing, not fixing. “For the first time, I could say ‘I’m struggling’ without someone immediately telling me what to do about it.”
This practice of being present without performing opened a door. She sought out spaces that allowed her to be curious about how she wanted to feel. She learned how to hold space, not giving advice or rushing to fix uncomfortable sensations in herself or others, but attending to them. It was encountering body neutrality through anti-diet advocate Christy Harrison, who “introduced neutral terminology… It sort of alleviated shame.”
Further transformation came through Suzie’s work with Indigenous communities on environmental guardianship. “When I started working with Indigenous people specifically on the business case for a First Nations National Guardians Network and with the Reconciling Ways of Knowing Stewardship Society…it helped me to see how everything, and I mean everything, is connected… It’s not just mental. It’s mental, physical, emotional, and spiritual health and well-being. And, we are all part of something much larger.”
The more Suzie was given space to practice what was present for her, the more she learned from others, and the more inspired she became to give to communities and engage with challenging intersections of meaning. She now practices trauma-informed dance and regularly teaches embodied movement practice, with an ongoing attention to how the body senses safety or benefits from any performance. That’s how we met, in 2022, as two people invited to learn a skill neither of us thought we could be known for: intentional, self-compassionate being with our bodies. “I need to listen to my body sometimes,” Suzie told me, “The physical is what moves the mental… I had separated the body and the mind.”
It’s the grounded and dynamic awareness that Neff’s research shows can be cultivated through self-compassion practice. She treats herself with the kindness she’d extend to a friend, recognizing that all bodies change and struggle, and practices different approaches to bring attention to what’s present (Neff & Germer, 2018). Suzie’s nervous system is still learning to trust. After years of being told that hunger meant weakness, her somatic responses carry those lessons. Now she’s found communities where different learning becomes possible—where bodies aren’t problems to solve but wisdom to honour.
I Know the Medicine Is Love
On our first night cooking at the community dinner, Theresa stood at the door to the dining area, nervously swivelling her gaze between the crowd quickly assembling and me, squatting in front of the oven. “Ten minutes, chef,” I said, giving her a smile.
One of the ovens had stopped working that afternoon—we’d only discovered that terrible truth 45 minutes prior. I had been rotating trays between racks with the working oven on high, and I could tell Theresa was settling a little, easing from the stress this dead oven had set off in us both. She turned to fully face me, waiting for my eyes to find hers. In the most neutral, kind voice she could muster: “Can you handle this? I’ll send out the veg.”
I saw how much she cared, saw her searching me for understanding. I gave her one certain, assured nod: “Ten and on the table!”
She trusted me enough to do my part, and that felt so affirming. I volunteered to help with the meal to prove to myself that I could still be reliable and capable of responding to others in dynamic situations, which I used to be great at. She gifted me with confidence and resilience, and this is what we’ve been practicing for three years now. We don’t aim for perfection; we focus on the process and staying present to what may be needed when things fall apart. We strive to notice the needs of the community and then extend Neff’s practice of self-compassion into collective space, treating mistakes as part of our common humanity rather than some evidence of individual inadequacy (Neff & Germer, 2018).
Theresa, the 70-year-old Chinese Canadian chef who shaped the community meal space, has had an unconventional and storied career marked by long hours, dignitary dinners, and teaching new chefs the professional way as a Red Seal instructor. She found herself in leadership roles wherever she landed. “I think in my younger days of being a chef…not being able to show my female side, I wanted to be as strong as every boy or man in this kitchen, whether he’s bigger, older or whatever. I have to be as strong or stronger to be considered any good,” (personal communication, interview, November 2, 2025).

Theresa in the community kitchen, finishing up the last of our work. Photo by Sheena Venditti, November 12, 2025. Collage images of the chefs and kitchens that inspired her, stock image by davit85, August 31, 2020, https://www.istockphoto.com/photo/restaurant-manager-and-his-staff-in-terrace-interacting-to-head-chef-in-restaurant-gm1268392517-372294954.
In 2018, two years from retirement, Theresa had long since learned to put on a tough face when she wasn’t feeling good enough. The day she got hurt, she was struck violently between the eyes when a poorly stored product slid from overhead and pinned her inside a walk-in fridge. Several heavy baking sheets fell into her face and on her head. The WCB later reduced the life-altering concussion to “got hit on the head with a half sheet of cookies,” a minimization that left Theresa battling for the meaning of her experience to be recognized.
Theresa’s story shows us what happens when bodies break down, and how institutional care’s best practices discount our felt experience. She described her symptoms clearly: stuttering, word-finding difficulties, and getting lost on familiar routes. Because her injury wasn’t visible, insurance officers treated her claims with suspicion.
Theresa was asked to fill out complex forms while cognitively impaired, to prove her injury over the phone to strangers who’d never met her, to return to work part-time while debilitating symptoms persisted because “treatment” meant proving she could function. Theresa wanted to function, so she forced herself to meet all the requirements in hopes that the effort would lead to effective treatment for her concerning symptoms.
Her nurse practitioner, Colleen, had been the only medical professional who honoured Theresa’s embodied experience – the only person in her medical team who had built a relationship with her. When Theresa came in, struggling to answer questions, repeating herself, behaving far outside her baseline functioning, Colleen immediately recognized what bureaucrats couldn’t see. Taken as a whole, it was clear that this person had been fundamentally altered. Later, helping Theresa fill out disability forms, Colleen put her arm around her: “How they expect somebody with a brain injury to do this is beyond me. Me and my colleague are smart women and we are struggling.”
For three years, Theresa had to perform and prove her reality, asking people to take her actual felt experiences seriously. By the time she was compensated fully, she’d lost her career and exhausted her savings. She was not recognized as having a brain injury by WBC standards, so she received no treatment for her condition. After decades of proving herself in professional kitchens, of never showing weakness, her concussion had forced a solitary reckoning with limits she’d spent a lifetime denying.
What began to shift for Theresa was finding spaces where her vulnerability could be witnessed without judgment, where her capacity was celebrated, and where her feelings were welcome. At church, the shared effort to be present to each person’s experience gave Theresa the chance to process her loss and begin making deep connections. This support inspired her to share more of herself. She started small, making soup and fresh-baked bread for community events. When we repeatedly experience genuine compassion: loving-kindness, recognition of our shared humanity, mindful presence, it’s possible for new patterns of relating to form (Neff & Germer, 2018).
When we met years later, Theresa had grown a small regular practice into two community meals a month, which feed around 100 people, and are supported by about 20 volunteers. The church community had seen her passion and wanted to support it. The leadership secured grants to allow Theresa to create a shared space where neighbours could sit, break bread, and take in one another’s company. Theresa brought professional expertise to the task. She knows how to organize a kitchen, teach knife skills, and scale recipes for crowds. Her community allowed her to develop practices that honoured her limits, and they all created systems that worked for the people who wanted to join. As she received more support, there was more that could be done for the neighbourhood – this collaboration with compassion created real community capacity.
I came into that space through a celebration of life; I had just gone to support a friend. When I saw the energy the group brought to their work and the total acceptance and embrace of their different abilities and needs, I had to find out how I could be part of it. I tracked Theresa down to give her my number and to ask her how I could work with them to create more moments like that.
Theresa’s been given a safe-feeling opportunity to teach, and she prides herself on checking in with all the participants, always embracing their feedback as essential to our shared success. Research on community capacity shows that trust is built through consistent, transparent engagement and shared decision-making (Lansing et al., 2023). The work we’re doing, chopping vegetables, learning the steps we need to take together, is trust-building; it’s how we cultivate community care.
Theresa still struggles with “glitches” in her cognition; she is still affected by the accident, as her brain injury makes managing her wellness difficult. She also has a special attention to what she has experienced, because of her community: “There’s a thing that happens in true healing. There’s a warm energy to it, different from your favourite slippers or cozy blanket. It’s a different warmth- it feels good, it tastes good, smells good, and it creates such a clarity of mind. I think that medicine is love. I know that medicine is love, especially when I came to Saint Stephen. It was that warmth. I walked into love.”
Gratitude and reciprocity, Potawatomi ethnobotanist Robin Kimmerer teaches, have the remarkable property of multiplying with every exchange, their energy concentrating as they pass from hand to hand, a truly renewable resource. (Kimmerer, 2020) This is true for community dinners and for movements. When we practice care in our immediate communities, we’re also developing the skills and relationships we’ll need to create the spaces we need, while experiencing gratitude and inspiring reciprocity.

The view from the parking lot: the community dinner entrance, framed by moments from the night; a pot being stirred top left, a busy dinning room at top right. Photos by Sheena Venditti, November 12, 2025.
Building Networks, Building Power
Holding my friends’ stories, I glow with pride at their work and growth. I recognize that I am living in spaces that allow me to be seen, that give me a positive social identity: a sense of belonging and meaning. Research on social identity and collective action reveals that people feel most inspired when they strongly identify with their group and believe in its effectiveness (Fritsche et al., 2018; Masson & Fritsche, 2021). We are all building something bigger than service, a strength that matters.
In community spaces, as we learned to find safety even when we felt vulnerable, by staying present when ovens broke, when people’s symptoms flared, when someone needed to sit down mid-task, we were also building networks. Theresa connected me to a mutual aid group organizing around food insecurity. Suzie introduced me to land recognition and shared ways I can become more involved in decolonizing work. I connect people to embodiment work.
The trust we built over chopping vegetables and washing dishes became the foundation for showing up together in other spaces: at neighbourhood meetings demanding accessible housing, at actions supporting healthcare workers, in mutual aid networks distributing food and resources. This is what organizers call “relational organizing”: building power not by mobilizing strangers but by deepening relationships with people we already know and trust (The Action Lab, 2024).
Community care isn’t separate from collective action: it’s a stage of it. When we practice staying present with each other’s vulnerability, when we learn to witness struggle without trying to fix it, when we build the capacity to hold our human complexity, we’re building the somatic and relational skills necessary for sustained organizing. Research shows that collective action happens when people experience intense emotion, strong group identification, and belief in collective efficacy (Jost et al., 2017). Our actions built all three.
The networks we create continue to expand what is possible for all of us. Theresa mentors young chefs to help them get their first jobs; she often reaches out to schools for mutual aid. Suzie is revising the policy for her nonprofit organization, SheRecovers, to better reflect body neutrality. I learned from both of them how to support others while honouring my own limits. We practiced what Hemphill teaches: that our bodies remember what our minds forget, and that how we show up together in small moments prepares us for how we’ll show up together in larger struggles (Hemphill, 2024).
We are building working systems outside economic exchange and bridging the trust gap that many people feel toward institutions. Survey data show that higher-income Canadians report much greater trust in doctors, scientists, and educators than those of lower economic status (Steinburg, 2024). This trust gap is a health equity issue. People with greater financial resources tend to trust that asking for support will secure what they need. This increased trust facilitates their access to care and social information. Lower levels of generalized trust can make it harder to access the co-regulation pathways that Porges describes, leading to less connection and support. According to Porges’ research, a long-term lack of safety—characterized by not feeling truly heard or recognized with a sense of acceptance—causes you to stop seeking it. You no longer scan for it, pursue it, or expect it (Porges, 2025). Pity, dismissal, and control create truly harmful distance. By creating spaces of connection through community care, we can give to one another what our institutions cannot. Each of us can choose to make safety feel more possible for one another.
Care builds capacity. Relationship creates resilience. When we center our actions in connection rather than isolation, fundamental transformation becomes possible- not just for individuals, but for the communities we create together. Practicing being together prepares us to move and transform together, so that the networks we weave across people we trust expand what is possible for all of us. Standing solid on my feet in that cold parking lot, I know this in my body: our interdependence is our strength.
References
The Action Lab. (2024, July). Power to Win. The Forge. https://cdn.prod.website-files.com/64ee1477f185f9ae19154371/66c73761b20758ef85cd1637_Power%20To%20Win%20Report.pdf
Barrett, L. F. (2017). How Emotions Are Made: The Secret Life of the Brain. HarperCollins.
Dobson, K. G., Chien, Y., Carnide, N., Furlan, A. D., Smith, P. M., & Mustard, C. A. (2024). Uncovering Mental Health Profiles of Workers with a Physically Disabling Injury or Illness Using the Complete State Mental Health Framework. Journal of Occupational Rehabilitation, 35(4), 929-944. https://doi.org/10.1007/s10926-024-10254-3
Epps-Addison, J. (2024, December 24). Reflection on the Power to Win Report: Organizing for a Just Future. The Forge. Retrieved November 29, 2025, from https://forgeorganizing.org/article/reflection-power-win-report-organizing-just-future/
Fritsche, I., Barth, M., Jugert, P., Masson, T., & Reese, G. (2018). A Social Identity Model of Pro-Environmental Action (SIMPEA). Psychological Review, 125(2), 245-269. https://doi.org/10.1037/rev0000090
Greif. (2023, July). Brain Injury Canada. https://braininjurycanada.ca/en/caregiver/mental-health-caregiver/grief/#:~:text=Loss%20of%20you%2C%20me%2C%20and,relationship%20after%20a%20brain%20injury
Hemphill, P. (2024). What it takes to heal: How transforming ourselves can change the world. Random House.
Huberman Lab podcast. (2023, October 15). How to understand emotions | Dr. Lisa Feldman Barrett [Podcast]. YouTube. https://www.youtube.com/watch?v=FeRgqJVALMQ
If you want to improve the world, start by making people feel safer. (2022, September 25). Trauma-Informed World. https://traumainformedworld.com/2021/11/24/if-you-want-to-improve-the-world-start-by-making-people-feel-safer/
Jost, J. T., Becker, J., Osborne, D., & Badaan, V. (2017). Missing in (Collective) Action. Current Directions in Psychological Science, 26(2), 99-108. https://doi.org/10.1177/0963721417690633
Kosse, F., Rajan, R., & Tincani, M. M. (2025). The persistent effect of competition on prosociality. Journal of the European Economic Association. https://doi.org/10.2139/ssrn.4634501
Lange, P. A., Kruglanski, A. W., & Higgins, E. T. (2011). Handbook of Theories of Social Psychology: Collection: Volumes 1 & 2. SAGE.
Lansing, A. E., Romero, N. J., Siantz, E., Silva, V., Center, K., Casteel, D., & Gilmer, T. (2023). Building trust: Leadership reflections on community empowerment and engagement in a large urban initiative. BMC Public Health, 23(1). https://doi.org/10.1186/s12889-023-15860-z
Leung, W. (2018, November 11). Canadian study finds major traumatic injury increases risk of mental-health diagnoses, suicide. The Globe and Mail.
Lewis, I., & Houdmont, J. (2024). “I’m pulling through because of you”: injured workers’ perspective of workplace factors supporting return to work under the Saskatchewan Workers’ Compensation Board scheme. Frontiers in Rehabilitation Sciences, 5. https://doi.org/10.3389/fresc.2024.1373888
Loehnen, E. (2024, June 4). Prentis Hemphill: Recovering Our Ability to Feel (TRAUMA) — Elise Loehnen. Pulling the Thread. Retrieved December 4, 2025, from https://www.eliseloehnen.com/episodes/h1mjtwhv3bo2nddnd6ikmoj8ogsbzf-8xa2s
Masson, T., & Fritsche, I. (2021). We need climate change mitigation and climate change mitigation needs the ‘We’: A state-of-the-art review of social identity effects motivating climate change action. Current Opinion in Behavioral Sciences, 42, 89-96. https://doi.org/10.1016/j.cobeha.2021.04.006
Mikołajczak, G., & Becker, J. C. (2019). What is (un)fair? Political ideology and collective action. Journal of Social and Political Psychology, 7(2), 810-829. https://doi.org/10.5964/jspp.v7i2.1230
Neff, K., & Germer, C. (2018). The mindful self-compassion workbook: A proven way to accept yourself, build inner strength, and thrive. Guilford Publications.
Porges, S. W. (2017). The Pocket Guide to the Polyvagal Theory: The Transformative Power of Feeling Safe. Norton.
Porges, S. W. (2021, August 1). Critical discussion of Polyvagal theory. Polyvagal Institute. https://www.polyvagalinstitute.org/vagal-paradox?gad_source=1&gad_campaignid=20399496868&gbraid=0AAAAABqScxoaoccyF_vgc8YbfzEYW0pCN&gclid=Cj0KCQiA0KrJBhCOARIsAGIy9wCpSys1QhknmZJ7T0l6uq7UsY6AS5KLtVx_fOLe9ddMkH7kF7WJutQaArBXEALw_wcB
Porges, S. W. (2025). Polyvagal theory: Current studies, clinical applications and future directions. Clinical Neuropsychiatry, 22(3), 83-93. https://doi.org/10.1016/b978-0-12-816996-4.00018-6
Post-traumatic stress disorder. (2024, May 27). World Health Organization (WHO). https://www.who.int/news-room/fact-sheets/detail/post-traumatic-stress-disorder
Rogerson, O., Wilding, S., Prudenzi, A., & O’Connor, D. B. (2024). Effectiveness of stress management interventions to change cortisol levels: A systematic review and meta-analysis. Psychoneuroendocrinology, 159, 106415. https://doi.org/10.1016/j.psyneuen.2023.106415
Rosa, G. (n.d.). Emotional anatomy. Giulia Rosa illustrations . https://stay-hop.com/collections/giulia-rosa-illustrations
Spitfyre, S. (2020, February 5). Inferno, Purgatorio, Paradiso (or Weigh-in Wednesday #3, Part 2 of the ongoing saga that is OMG…what if I don’t have a pretty face?). OMG…what if I don’t have a pretty face?. https://whatifidonthaveaprettyface.blogspot.com/2020/
Stangor, C. (2016). Social Groups in Action and Interaction. Routledge.
Statistics Canada. (2024, August 15). Trust in News or Information from Media by Gender and Other Selected Sociodemographic Characteristics. Canada. https://www150.statcan.gc.ca/t1/tbl1/en/tv.action?pid=4510009701
Steinburg, J. (2024). Trust in Canada: Recent Trends in Measures of Trust. Trust in Research. (TRuST) Scholarly Network Undertaken in Science and Technology. https://uwaterloo.ca/trust-research-undertaken-science-technology-scholarly-network/sites/default/files/uploads/documents/trust-in-canada-recent-trends-in-measures-of-trust-april-2024.pdf
Stroebe, K., & Postmes, T. (2019, July). Where Did Inaction Go? Towards a Broader and More Refined Perspective on Collective Actions. PMC Home. Retrieved November 29, 2025, from https://pmc.ncbi.nlm.nih.gov/articles/PMC6619099/#bjso12295-bib-0022
Suzie Spitfyre looks forward to a new lifestyle. (2013, April 17). Victoria Times-Colonist. https://www.timescolonist.com/archive/suzie-spitfyre-looks-forward-to-a-new-lifestyle-4586211
Wall Kimmerer, R. (2020). Braiding Sweetgrass: Indigenous wisdom, scientific knowledge, and the teachings of plants. Penguin Random House Canada.
Wall Kimmerer, R. (2022, October 26). The Serviceberry: An economy of abundance – Robin wall Kimmerer. Emergence Magazine. https://emergencemagazine.org/essay/the-serviceberry/
Watts, R. (2014, January 6). Health challenge devotee Suzie Spitfyre sets new goals. Just a Moment.. https://www.timescolonist.com/archive/health-challenge-devotee-suzie-spitfyre-sets-new-goals-4603927
Watts, R. (2014, January 6). Health challenge devotee Suzie Spitfyre sets new goals. Times Colonist Victoria. https://www.timescolonist.com/archive/health-challenge-devotee-suzie-spitfyre-sets-new-goals-4603927
